Are you living with Diverticulitis or Diverticulous? If so, this article may answer some of your concerns. Been there, done that.
Introduction
First off, this article is a minor divergence from the rest of my posts, because it is about a different pain. Some of the related articles apply here. Others do not. But because it does deal with pain, and because I have been living with diverticulitis for some time now, I knew it was important to write about.
So if you are living with this problem, and want to know more about it from a non-medical person, than this is your article. I have spent time researching, applying what I have learned, and in the hospital for surgery. It is my hope that you will find some answers here that might help you with this disease. I want to emphasize I am just a fellow sufferer, so please use this article for reference only. If you have this problem, see a doctor. Things could get serious.
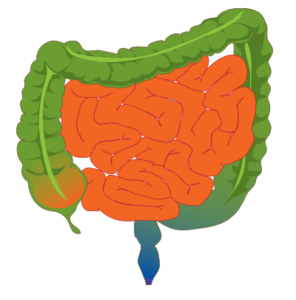
Diverticulitis
So what is diverticulitis? According to WebMD, it is an inflammation or infection of small pouches called diverticula that develop along the walls of the intestines. From my research and talking with doctors there are no known indicators of why these occur. As we age there is an increase in this happening. Genetics seems to play a part. My paternal aunt suffered from it; which I found out when I had my most recent occurrences. Click this link to see an image of what I am describing. I couldn’t find one to show you that I could use legally.
Different from Diverticulosis
What is diverticulosis? I heard this term bounced around like I was supposed to know what it meant. Which I didn’t. The definition of diverticulosis is when the diverticula form in the pockets of your intestines. Apparently this isn’t a problem unless they become inflamed which is what diverticulitis is. Generally a person doesn’t know they have diverticulosis because there aren’t any symptoms. Diverticulosis is usually diagnosed from a sigmoidoscopy. The doctor can see if the diverticulum (singular) or diverticula (plural) have formed.
Symptoms
Pain. In my experience, a cramping ache; not super acute but uncomfortable nonetheless.
Other symptoms might be; vomiting, constipation, nausea, and even bleeding from your rectum. Of course if there is bleeding get to the doctor now.
Take your temperature. Watch for dehydration. (Did you know a simple test for checking if you are dehydrated is to grab/pinch the back of the skin on one hand between the thumb and forefinger of the other? If the skin doesn’t go back to original flatness right away you are probably dehydrated. See a doctor.)
Here is a good article about the illness from Physiopedia. This article includes more symptoms.
Diet
This has been the most frustrating part of this experience. When I was in the hospital in June 2019 I asked every health care professional what sort of diet I should be following. I did this because I am very proactive about my health. I truly wanted to avoid having this problem. Here are some of the answers: nothing spicy, low fiber, high fiber, nothing fried. What the heck?
There is confusing information on the web too. The general information isn’t that helpful. The old wisdom was to avoid seeds and nuts. That isn’t the case anymore.
So I figured I would ask my gastroenterologist. After all, he knows intestines! This appointment was a followup after my hospital stay in June. In the hospital I had been told there would be a possibility of removal of part of my colon, where the infection was. And the possibility of an ostomy bag.
The gastro doctor was circumspect about the surgery; he said how much colon can you remove? I liked this attitude. If there was something I could do about it myself, then I was motivated. So I asked what I should be eating. His answer was first a lesson.
He said that diverticulitis was not a known disease until man started to mill grains. After that, it appears on the scene. And countries like Asia and Africa that don’t eat lots of milled grains have less incidents of it. So, he basically told me to cut out grains including wheat, corn, and rice. He also recommended not eating potatoes. He said quinoa was okay. No fried foods.
Now I had been avoiding wheat because gluten gave me cramps and diarrhea. But I love corn and eat rice and potatoes. But if I can avoid any further bouts of this disease I will not eat those things.
He said a high fiber diet is good because it moves things through the intestines. So I am eating mostly fruit, vegetables, and protein. I’ve lost weight. Which is a good thing as I needed to. But not this way!

There is also a recommendation to avoid alcohol. Alcohol irritates the lining and you want your lining as healthy as possible. This wasn’t a problem for me to not drink; I avoid alcohol.
So I followed the advice as best I could, but the infection never went away completely. After consults with a few doctors, including the gastro doc, surgery was recommended.
My experience
You can skip this section unless you want to read about what happened. It might be helpful to you to decide what you should do. Like learning from my mistakes.
This problem put me in the emergency room about four years ago. I thought I had the flu. I kept throwing up, had chills and my stomach hurt. Mistake number one; I didn’t monitor my temperature. If I had, I would have realized I was very sick. I went to Urgent Care on a Saturday. They gave me IV fluids and sent me home. (I don’t think they should have sent me home.) Sunday I was no better, and since Urgent Care wasn’t open, I went to the ER. Being it was a county facility, it was busy, but bless that staff, within 15 minutes I was admitted. They recognized how sick I was. Diagnosis; diverticulitis with a secondary urinary tract infection and border sepsis. That sepsis can be fatal! (It was a primary complication in Christopher Reeve’s death.)
What I learned from this experience is to monitor my temperature. I bought a thermometer. Whenever I get sick I track my temperature. Temperature is a good indicator of how sick you are. Get to a doctor if it is above 100 degrees. See this article for more about your temperature; At What Temperature Should You Actually Start Worrying About a Fever? And check to see if you are dehydrated. If you are throwing up, chances are you will become dehydrated. This is dangerous and should also take you to the doctor.
Fast forward to 2019. Recognized the symptoms in January. Went to the doctor. Prescribed antibiotics. Completed. Felt OK for a week. Recognized the symptoms in February. Ditto, ditto, ditto, ditto. Felt okay March and April. Recognized the symptoms in May. Ditto x 4. And again in June, the same.
But this time the doctor was concerned that I wasn’t getting better so she referred me to get a CT scan. I spent the afternoon in the Imaging and Urgent Care departments, to finally be told that there was a possible cyst/growth/infection in my diverticula and they wanted to admit me to the hospital. Spent another six hours in the ER, waiting for a bed. (I am not here to complain about the hospital or my care. They just didn’t have any beds. All my caregivers were wonderful. I received excellent care.) Spent 3 days in the hospital on IVs and antibiotics.
Discharged with an IV line in me to administer antibiotics in hopes of killing the infection. After a month of that, the infection was still present and there was worry of it attaching to my bladder. Surgery scheduled for September. I was on antibiotics for three months, just to keep the infection at bay. Successful laparoscopic surgery 14 days ago, where they removed about 10 cm of my colon. I am not allowed to drive yet, or to take a bath. I can shower.
Recovery is to walk everyday, a little more each day. Apparently moving around can help the gastro-intestinal system move too. Movement and exercise are things I have been promoting in my other articles for pain management. See one of my articles here.
All this is to say that this illness can really impact your life! And my advice is to keep really vigilant about your health. I should have asked to have a CT scan after the second bout in February. But I didn’t know any better. I didn’t have a fever after all. But you should learn from my mistakes. Advocate for yourself. Do research. Find a doctor that will advocate for you.
If You Have Surgery
My surgery was the best of all possible outcomes. The surgeon said it went really well. (I did everything to the letter to prepare; fluids only, drink that disgusting GoLytely stuff that cleans you out.) I didn’t have to get an ostomy bag.
Pain was minimal at the 3 incision sites. More pain from the gas that they pump into you. Each day the pain was less. I was on clear liquids for a day, then regular food. There was a multi page packet sent home with me with what I could and couldn’t do. The instructions recommended a low fiber diet. But I had already started my high fiber in the hospital and had no problems, so I stuck with that. (Here again, there is no consensus.)
Something You Can Do In the Meantime

One product the Gastroenterology doctor did recommend was Citrucel.
He said he likes it best because it helps both constipation and diarrhea. I have recommended it to a friend who has trouble with constipation and it has helped him.
Here is a picture I took of my bottle. You can get it in powder form too. If you click on the link for the powder form, I receive a referral fee.
Are You Interested in Building Your Own Website?
If you, like me, are limited in your ability to work or go to a job site, building an income producing website might be an option for you. I am using the Wealthy Affiliate platform. You can join for free to see if this might be an opportunity for you. If you do become a member I will receive a referral fee. I will also be your mentor and help you as much as I can. Click here to check it out.
Conclusion
What about you? What has been your experience with this disease? Did this article answer your question? I would like to know any positive or negative feedback. I want this article to help those of us who suffer from this.
Please leave me a comment. You will be helping me and others. Thank you.
